Mennonite Health Journal
Articles on the intersection of faith and health
Mennonite Health Journal, Vol. 19, No. 6, November 6, 2017
PDF version
Student Elective Term Report
Moi Teaching and Referral Hospital, Eldoret, Kenya
August 29- October 8, 2017
Matthew Glick
I tend to be a very structured person. I’ve eaten the same lunch every day for the last four years. I often get frustrated when my plans get changed at the last minute. And when I get stressed or busy I plan my week out down to the minute to ensure no time is wasted. All this to say, if you were building a personality that would fit best in the Kenyan medical system, it would be someone who is flexible, easy-going, and thrives in uncertainty–the exact opposite of mine.
When I think back on my time in Kenya, the overarching theme has been this uncertainty. This theme was no doubt helped by the Kenyan Supreme Court annulling the results of the presidential election on the day I arrived, shocking the world and throwing my trip in flux for the first three weeks I was in Kenya. The theme of uncertainty followed me throughout my time in Kenya, both in the wards and in my experiences throughout the country, as if God had decided that my desire for order and reliability at home needed to be thrown in the garbage. Through this uncertainty, I’ve learned to adapt my clinical style and relearned the freeing feeling of being wholly present in a moment.
I spent a little over five weeks working at the Moi Teaching and Referral Hospital (MTRH) in Eldoret, Kenya, the fifth largest city in Kenya and supposedly the fastest growing city in East Africa.
My second week on the adult medicine wards, I admitted a patient transferred from another hospital for severe malaria. She had been receiving treatment at a regional center when she developed cola-colored urine and then stopped making urine all together.
Normally, when receiving a patient from an outside hospital in the States there is some degree of confusion and uncertainty. Sometimes one isn’t completely sure exactly what workup and treatment has been done, and generally one feels less on top of the patient’s management than if you had admitted them from the beginning. However, usually patients come with a big packet of all their previous labs and maybe write-ups of imaging results. As a med student I’ve had the pleasure and responsibility of sorting through these packets to find pertinent information as the team tries to take control of the patient’s care.
As can be imagined, this process is made much more difficult in Kenya, with no EMR systems and no packet of previous lab tests and treatment sheets. Essentially the patient was just “there” on rounds one morning, laying in bed next to another patient. Making this process even more uncertain in this case was the fact that the patient spoke Turkana, a tribal language not spoken by any of the medical team and certainly not by me. Therefore, communicating with her required the use of a different patient’s family member who happened to speak the same language, and the translation of my English to Swahili to Turkana, and back again. Because of the general lack of information both from the referring hospital and from the history, we essentially had to start the medical process over again, checking a malaria smear, getting basic labs, and having to take the patient’s word about what medicine she had received at the outside hospital. Once we had established that she did indeed have malaria, and her kidneys had been injured either due to the malaria or the treatment she was given, we were able to form our treatment plan, artesunate for the malaria and fluids to try to help her kidneys recover.
Simple enough–that should be the end of all the confusion. However, one thing I learned having worked at MTRH is that you can rarely trust that something happens unless you see it happen. The patient to nursing ratio often pushes 20:1, so things like fluids, medications, and imaging sometimes get overlooked. As a wet-behind-the-ears med student who is used to orders getting done like magic when I enter them into the EMR, I had no idea that I needed to micromanage this patient’s care more than any before. It wasn’t until three days later, when the patient was still not making urine despite having supposedly received nine liters of fluids, and showing no signs of fluid overload, that it occurred to me to ask the patient’s family member if she was getting the prescribed fluid each day. She informed me she had gotten about one and a half liters in those three days. Due to the difficulty in communication, I hadn’t thought to ask if our treatment plan was even being followed. I then learned the MTRH trick of giving the bags of normal saline for the day to the family member, and making sure she alerted the nurse to hang a new bag when the last one was finished. Involving family members heavily in the patient’s care is crucial at MTRH when the nurses are overworked and the infrastructure of delivering medication is non-existent.
My patient eventually recovered kidney function and was discharged. I learned valuable lessons from caring for her and in subsequent encounters in Kenya. The first lesson was that I needed to increase my involvement in patient care. As a medical student, I’ve been able to be ignorant about if parts of patient care actually get done rather than just talked about. On most rotations in the States, I can present a plan on rounds and my labs and medications “magically” get ordered by the intern or resident. As I’ve progressed throughout my clinical years I’ve recognized the need to verify that things happen more and more, but I was not prepared for the level of medical oversight that is required in Kenya. In order to provide what I considered adequate care, I needed to essentially micromanage my patients, verifying that every single test and treatment that we prescribed was completed. This awareness will be vital as I proceed forward into residency and beyond, when there is no longer a safety net to catch things that I let fall through.
Secondly, I learned how to be adaptable in delivering medical care. This adaptability started with my realization of the need to have the patient’s daughter make sure the proper amount of fluids were delivered, but did not stop there. I learned that a catheter bag and IV tubing makes a perfectly acceptable way to drain ascites fluid while still measuring the volume. I gained an amazing appreciation for the physical exam skills of my Kenyan colleagues. In times where I would normally ask for an ultrasound, CT, or more lab tests, they were able to use the physical exam to find ascites to tap, measure the size of the spleen, or check a patient for anemia. In this resource-limited setting it is immensely valuable, both to the patient and the clinician, to be able to find shifting dullness or a fluid wave instead of ordering an abdominal ultrasound, or to use percussion instead of bedside ultrasound to find the proper place to stick a needle for a thoracentesis. Sir William Osler said, “The practice of medicine is an art based on science,” and I was able to grasp that aspect of medical practice through this experience. Too often, medicine for me has felt pre-programmed, almost as if once I’ve treated one patient with CHF, COPD, or an AKI I’ve treated them all, but clearly that is not the case. I appreciate how the physical exam can help reduce patient cost by avoiding expensive imaging and redundant lab tests, and I can truly see now the art of medicine found in the physical exam.
Unfortunately, the variability of medicine in Kenya, while forcing me to adapt and become more resilient in my treatment plans, also can be extremely frustrating and depressing. My first day on the adult medicine ward we admitted a 40-year old female whom we eventually diagnosed with HIV/AIDS and pneumocystis pneumonia, an opportunistic infection that occurs when HIV has lowered a person’s immune system past a certain level. We began the typical treatment of oral antibiotics, but unfortunately over the course of the next week she continued to deteriorate to the point where she developed altered mental status from respiratory failure and infection. Normally in the USA we would have been able to go to the second and third line therapies once we had identified that she had failed the first line treatment, but both of those were not available at MTRH so there was nothing left to do. It was gut-wrenching to watch her slowly day-by-day dying on the wards over the course of two more weeks, with no ICU bed to which to transfer her and no other medications to give her. I can’t say that she would have survived in the US, since she was already pretty sick when she came in, but the difference in how aggressive we were able to be in giving her a fighting chance was extremely frustrating.
The uncertainty that permeated my entire trip was undoubtedly a good thing for me personally and for my development as a doctor. I learned more about the art of medicine through developing my physical exam skills and how one must be adaptable to make sure patients receive the best possible care. The difference in medical infrastructure pushed me to be more on top of my patients’ care, a realization that will absolutely benefit me as I go forward in residency and receive more responsibility. I was able to make friends with many Kenyan students with whom I lived in their medical school dorms. I had some great experiences both on and off the medical wards hanging out with the team. At those moments I would almost forget I was in Kenya! The interaction between team members on a medical service is universal, a strange mix of academic rigor, lighthearted joking, with the underlying awareness of the immense opportunity we share to have another person’s health in our hands.
Photo Gallery
MoiHospital
Moi Teaching and Referral Hospital is one of two referral hospitals in Kenya, and the site of Moi University Medical School. It also serves as the biggest cancer and chronic disease center in Western Kenya and the site of the AMPATH consortium, a partnership between Indiana University and about five other US medical schools with Moi University.
Moi-rounds
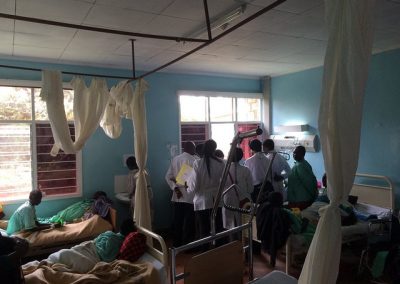
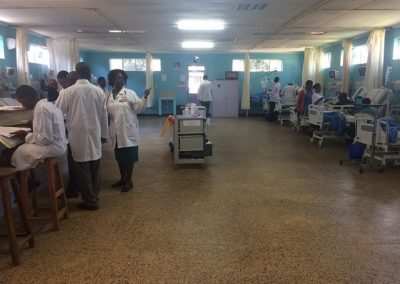
A typical day on rounds. Medical teams consist of one registrar (equivalent of a US resident), one intern, and 4-5 medical students. Twice a week a consultant (attending) comes in to round on patients with the team. The wards are very crowded, each team carries about 30 patients and patient often share a bed with another patient. The majority of my time was spent on the adult medicine wards, which are divided up into a male and female side.
Moi cardiovascular
The Cardiovascular Care Unit is a special unit specifically devoted to cardiac patients who need more intensive monitoring. They have eight beds but no ventilators so that the beds aren’t taken up by chronic ventilator-dependent patients. One of the biggest considerations at Moi is allocation of resources, with only a five-bed ICU, the ICU team has to be very pragmatic about which patients to accept. Every chronic ventilator-dependent patient they accept means one less bed for a patient with an acute issue that may be savable. I spent a couple days rounding with the CCU team before going to cardiology clinic.
Iten-Kenya
I spent most of my weekends in Iten, Kenya, about 45 minutes from Eldoret. Iten is at about 8000 feet elevation and on the edge of the Great Rift Valley, giving it the amazing views seen here. Because of the altitude and hilly terrain, it happens to be the home of most of the great Kenyan distance runners and there are various training facilities scattered throughout the city.
About the author
 Matthew Glick is a fourth-year medical student at Indiana University School of Medicine in Indianapolis. He plans to train in Internal Medicine and specialize in Pulmonary Critical Care. He is a 2014 graduate of Goshen College where he played basketball and majored in chemistry and molecular biology. Aside from medicine, he enjoys running, traveling, and biking.
Matthew Glick is a fourth-year medical student at Indiana University School of Medicine in Indianapolis. He plans to train in Internal Medicine and specialize in Pulmonary Critical Care. He is a 2014 graduate of Goshen College where he played basketball and majored in chemistry and molecular biology. Aside from medicine, he enjoys running, traveling, and biking.